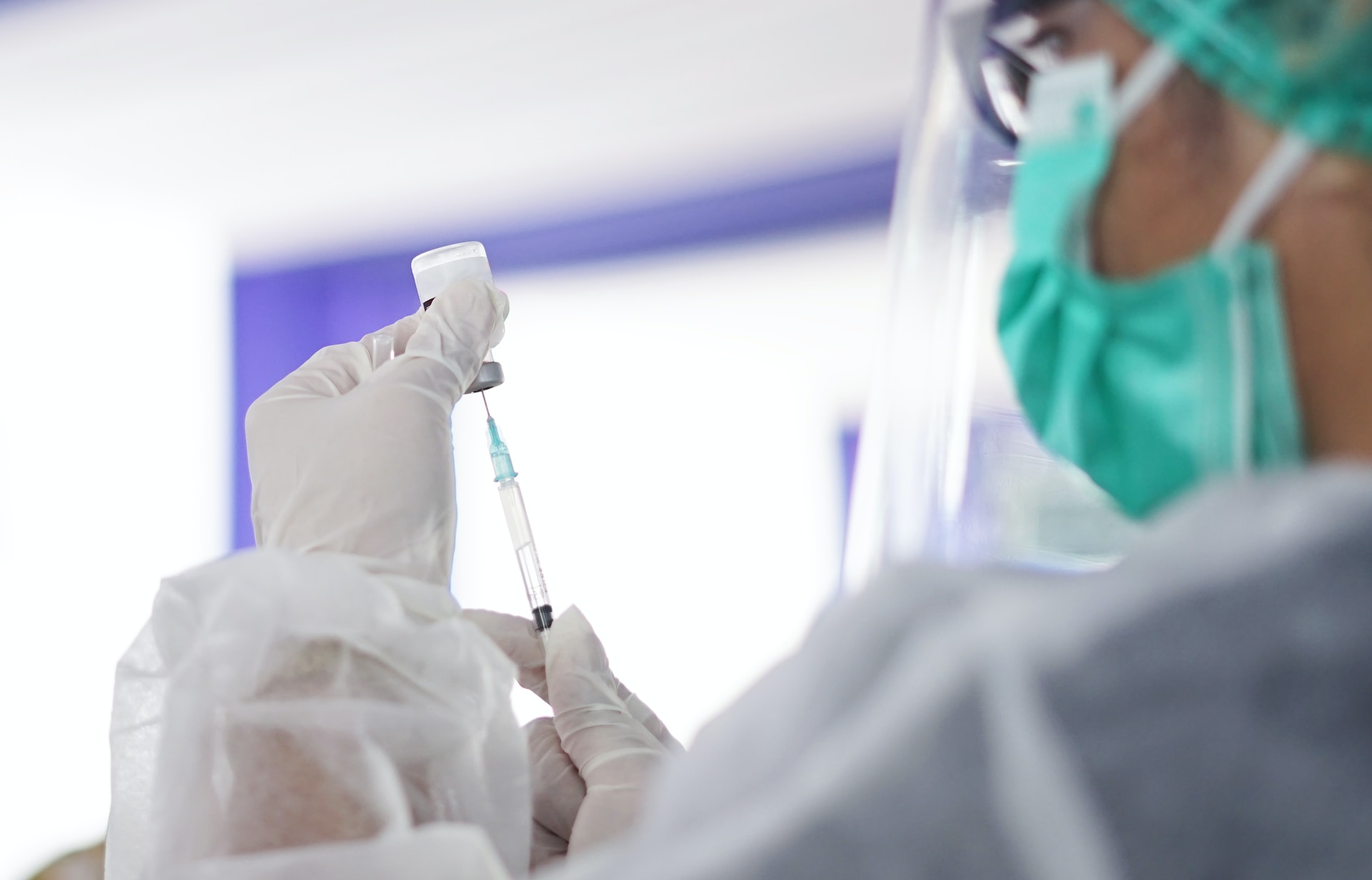
Scientists can create vaccines against infectious diseases with mRNA. The molecule instructs cells to build proteins that match parts of the pathogen, such as the spike protein from coronavirus. mRNA is typically packed into lipid nanoparticles to increase stability and cellular uptake. Several mRNA formulations have been optimized to maximize protein translation and modulate innate immune responses.
Contents
Regenerative Medicine
In regenerative medicine, we’re looking for ways to regenerate lost or damaged cells and tissues to replace the old or diseased ones. It has the potential to dramatically improve our quality of life and eliminate many incurable diseases. For this reason, scientists are excited about mRNA technology in the context of regenerative medicine. As a tool for growing tissues and organs in the lab and implanting them to restore lost function, mRNA technology holds tremendous promise. It also offers new opportunities to reduce the inflammation that leads to disease and target various genetic diseases with mRNA. In the early 1990s, researchers found that mRNA could instruct cells to produce proteins. They theorized that if they could alter mRNA’s four building blocks (nucleosides) so that it flew under the radar of the body’s immune system and no longer caused inflammation, they would be able to deliver a sequence of genes into the cells and order them to make any desired protein. This new technology would be ideal for creating autologous cell therapies and regenerative treatments made from the patient’s cells.
Vaccines
Vaccines train the body’s immune system to attack disease-causing pathogens. In a vaccine, an mRNA molecule instructs the cell to make a specific protein to help the body fend off or destroy a particular infection.
Over two decades ago, scientists realized that mRNA could be used as the basis for a new class of vaccines. They discovered that in vitro transcribed mRNA injected into cells produces proteins that can elicit an immune response. Unlike plasmid DNA and subunit protein vaccines, mRNA does not have to be inserted into the host cell’s genome to initiate protein translation; it simply enters the cytoplasm to trigger the production of encoded protein. Furthermore, mRNA can be delivered with minimal genetic vector, thus eliminating concerns about insertional mutations and the need for adjuvants, reducing vaccine delivery costs, and enhancing safety. The potential for mRNA-based vaccination is so great that investment in this technology is reaching epic proportions. In an early proof-of-concept study, mRNA molecules were injected into the hearts of mice with congestive failure; they instructed immune cells to break up and clear out the fibrosis.
Immunotherapy
Scientists worldwide have been dreaming about the infinite possible applications of mRNA as a drug platform. mRNA can deliver protein encoded by the genome to bypass the cellular machinery that usually produces the proteins, thus eliminating the risk of insertion mutations. Moreover, mRNA can be manufactured through IVT and non-invasively trigger protein translation. In addition, the mRNA-encoded proteins can be secreted to act in an autocrine or paracrine fashion, and they can also be loaded onto major histocompatibility complex (MHC) molecules, which can then present the peptide epitopes of the encoded protein to effector cells, leading to an immune response. Moreover, the immunomodulatory effects of mRNA are comparable to those of anti-drug antibodies. mRNA vaccines can be used to prevent infectious diseases and their variants, including new emerging pathogens, or for targeted cancer immunotherapies that activate the patient’s immune system to destroy tumors. IVT mRNA has been shown to enter cells of non-fenestrated tissues through micro capillaries and in mitotic cells through the cell layers adjacent to the capillaries. mRNA also reaches target cells in fenestrated tissues by transfection and a tetramer-mediated mechanism. In contrast, siRNA cannot cross the blood–brain barrier or act inside the brain.
Gene Editing
Messenger RNA, or mRNA, is a natural molecule manufacturing proteins in living cells. Researchers have discovered that mRNA can be programmed to act as a genetic instruction manual, making it possible to correct mutations at specific locations in genes to treat disease. In recent years, a new class of genetic tools called CRISPR-Cas9 genome editing systems has made modifying genes in cells and organisms much more manageable. CRISPR-Cas9 enables scientists to quickly and easily create cell and animal models for studying diseases and to develop therapies that change disease-causing mutations. Until recently, the technology was too expensive to be considered for use as a vaccine platform. However, the urgency to protect people against the COVID-19 pandemic catalyzed a breakthrough in mRNA-based vaccines and has ushered in a new era of democratized access to cutting-edge medical advancements. The mRNA-based vaccine platform uses liquid nanoparticles (LNPs) to deliver mRNA gene editing tools to human hematopoietic stem cells, or HSCs. LNPs are highly effective at protecting mRNA from degradation, crossing biological barriers, and efficiently delivering mRNA into cells for protein expression. They are now the delivery mechanism of choice for two leading mRNA-based COVID-19 vaccines in clinical trials and preclinical studies.